Driven by “pandemic fatigue” and Thanksgiving gatherings, COVID-19 case numbers and hospitalizations have surged in Los Angeles County to unprecedented levels. During the last week of November, the County logged an average of about 5,900 new cases a day; on Dec. 16, that number nearly quadrupled. Other metrics like hospitalizations and deaths lag behind case numbers, and the County has started seeing a precipitous rise in both. Since Nov. 9, average daily deaths have shot up nearly 600 percent, from an average of 12 per day to more than 70. Just before Thanksgiving, hospitals admitted nearly 300 new patients with the Novel Coronavirus a day; now, the County is seeing 600 new patients a day requiring hospitalization. All of this has public health officials eying the upcoming Christmas holiday with dread.
But as hospital and ICU capacity fill up, Christmas has come early to healthcare workers and residents of assisted living facilities in the County. This week saw the arrival of the new Pfizer COVID-19 vaccine to hospitals around the County, fresh from the company’s manufacturing plant in Kalamazoo, Michigan. Nine designated sites in Los Angeles County have received an allotment of the vaccine. Each site is equipped with the ultra-cold storage facilities necessary to keep the vaccine viable. Those sites will then send the vaccine to 83 acute-care hospitals across the County, including UCLA, Providence St. John’s, Children’s Hospital Los Angeles, and Cedars-Sinai. Major healthcare providers such as UCLA Health, Children’s Hospital Los Angeles, and Cedars-Sinai have started inoculating frontline medical staff, marking what experts hope is the beginning of the end of this pandemic.

“I am incredibly excited to be among the first group of healthcare workers to be offered the vaccine,” Dr. Sam Torbati, co-chair and medical director of the Ruth and Harry Roman Emergency Department at Cedars-Sinai, said in a statement. On Dec. 17, Torbati became one of the first in the County to receive the highly anticipated vaccine. “The vaccine gives us an additional, invisible shield and layer of protection.”
Along with Torbati, Cedars-Sinai has offered the vaccine to workers in the ICU and Emergency Department. The hospital notes that the vaccine is voluntary.
The Food and Drug Administration (FDA) granted emergency authorization to the Pfizer-BioNTech coronavirus vaccine on Dec. 11. The authorization followed extremely positive results from a trial of the vaccine, which showed a 95 percent effectiveness in preventing COVID-19. The vaccine requires two doses, given three weeks apart.
“The FDA’s authorization for emergency use of the first COVID-19 vaccine is a significant milestone in battling this devastating pandemic that has affected so many families in the United States and around the world,” FDA Commissioner Dr. Stephen Hahn said in a statement. “Today’s action follows an open and transparent review process that included input from independent scientific and public health experts and a thorough evaluation by the agency’s career scientists to ensure this vaccine met FDA’s rigorous, scientific standards for safety, effectiveness, and manufacturing quality needed to support emergency use authorization.”
Even as cases and hospitalizations surge, placing additional stress on an already-taxed healthcare system, Torbati says that the vaccine’s rollout holds promise to blunt the edge of the pandemic.
“This gives me great hope,” Torbati said.
This same sense of hope pervaded the Ronald Reagan UCLA Medical Center on Dec. 16, where mylar balloons and applause marked the first injections of the two-part vaccine. Emergency physician Dr. Medell Briggs-Malonson, the first at the hospital to receive the dose, described feeling optimistic.
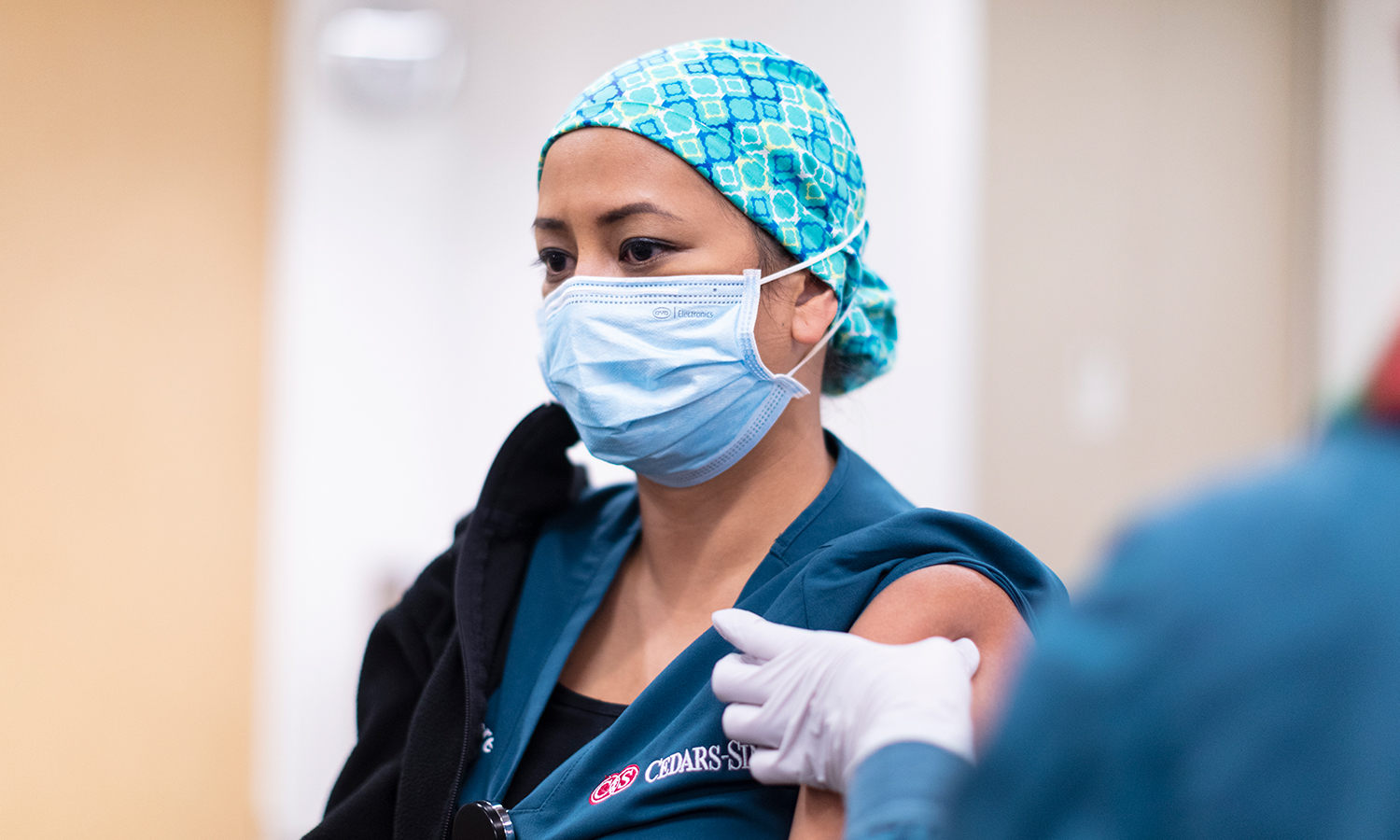
“I had a couple of butterflies, but then actually coming down and really realizing this was going to be the first shot and the first vaccine and then we can hopefully start to return to normalcy, it took all the flutters away,” she said in a statement. The next in line, nurse Nicole Chang, did not share Briggs-Malonson’s initial reservations. “I was like, ‘Please, let me go first! I’m so excited,'” said Chang, who works in the COVID-19 unit at UCLA Health Santa Monica Medical Center. In all her enthusiasm, Chang said she barely felt the vaccination itself. “It felt like nothing. I didn’t even feel a pinch!” But reflecting the trauma experienced by frontline healthcare workers in this pandemic, she noted the relative costs of a pinch against the virus. “A pinch is nothing compared to what these people go through [with COVID-19],” she said. “I’ve seen the devastation it causes.”
St. John’s Hospital, which is managed by the healthcare administrator Providence, has also begun the vaccination process. “This is a major scientific milestone that will help us to curb the spread of a disease that has brought the world to a standstill,” said Dr. Rod Hochman, president and CEO of Providence. “We are working to get the vaccine to the frontlines as quickly as we can, starting with our highest risk caregivers.”
Still more good news greeted healthcare providers as they administered the first doses of the vaccine across the country. On Dec. 16, the FDA acknowledged reports that Pfizer’s five-dose vials seemed to hold even more doses. While vaccines will commonly contain slightly more than the advertised dosage to guard against spillage or error, the reports indicated an even greater excess in Pfizer’s vials. In a discovery worthy of Hanukkah, some vials provided six, even seven doses, potentially expanding the nation’s limited supply by millions of doses.
“At this time, given the public health emergency, FDA is advising that it is acceptable to use every full dose obtainable (the sixth, or possibly even a seventh) from each vial, pending resolution of the issue,” the agency said in a tweet.
On Dec. 17, an FDA advisory panel of outside doctors and immunologists issued an endorsement to the FDA to grant emergency use of the vaccine produced by Moderna. The FDA is expected to grant the emergency authorization as soon as Dec. 18.
The second vaccine will be welcomed news in the Southland. On Dec. 17, intensive care units around Southern California reached a grim milestone of 0 percent capacity.







